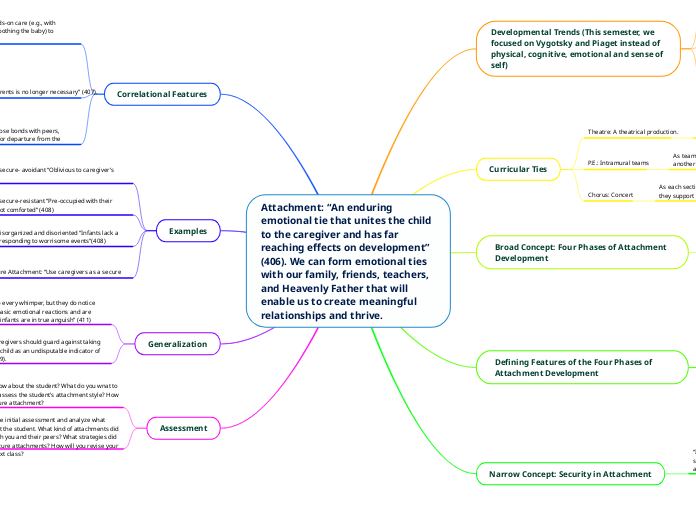
Hyperbaric Oxygen Therapy
Hyperbaric Medicine II
Hyperbaric oxygen therapy (HBOT) involves the intermittent inhalation of pure oxygen under a pressure greater than one atmosphere
Non-Diving Illness
Complications and Side EFfects
Claustrophobia
Approximately one out of 50 patients exhibit some degree of confinement anxiety in multiple chambers
rarely severe enough to require sedation
Mono-place chamber can be very anxiety provoking
Approximately one patient in 10, using the 25- inch mono-place chamber will have claustrophobia severe enough to make treatment difficult or impossible
Dental problems
Rarely, patients will suffer tooth pain during compression or decompression
Typically caused by an air space under a filling or restoration
Compression forces the pulp into the air space which causes exquisite pain
Lens Refractive Changes
Myopia worsens, presbyopia improves
Due to alteration in the shape of the lens
not cornea
Cause of shape change not known
Usually resolves completely following HBOT
some individuals refractive error may not completely revert to its pretreatment level
rare
It has been suggested, but not proved, that preexisting cataracts mature more rapidly with HBOT
Serous Otitis
May result from daily HBO
Usually minor problem
Treatment: decongestants
Finger Numbness
After 20 or 30 HBO treatments some patients complain of numbness in the fingers
Usually ulnar distribution
Disappears 4 to 6 weeks after therapy
Mechanism unknown
Pulmonary Oxygen Toxicity
Substernal chest pain, cough, and patchy atelectasis
May occur but is usually not seen if treatment protocols are adhered to
O2 Seizures
May occur particularly when HBOT is given at more than 2.4 atm
Some patients are idiosyncratically susceptible to high O2 partial pressures
Treatment: discontinue of the O2
Incidence of seizure is low
1.3/10,000 treatments
Sinus Squeeze
Occurs if any of the openings to the various sinuses to the head are blocked by an overgrowth of tissue, edema, or mucus
Very painful and the patient should undergo slow compression.
Decongestants
Round Window Blowout
Extremely rare complication caused by the vigorous performance of the Valsalva maneuver
Usually reported in divers
Very rare in a clinical hyperbaric patients
Normally, in an unconscious patient, the tympanic membrane ruptures before the round window gives way
Round or oval window blowouts usually produce immediate deafness, tinnitus and vestibular symptoms such as nystagmus and vertigo
2 Possible Mechanisms
implosive
explosive
Explosive Theory
When a diver attempts to clear a blocked middle ear space by performing a Valsalva maneuver and the eustachian tube is blocked a dramatic increase in the intracranial pressure occurs
Since the fluids surrounding the brain communicate freely with the inner ear fluids, this pressure may be transmitted to the inner ear
A sudden rise in the inner ear pressure could then cause the round or oval window membrane to explode
Implosive Theory
During descent pressure is transmitted from an inward bulging eardrum, causing the ossicles to move toward the inner ear at the oval window
This pressure wave is transmitted through the inner ear and causes an outward bulging the round window membrane
If a diver performs a forceful Valsalva maneuver and the eustachian tube suddenly opens, a rapid increase in middle ear pressure occurs. This causes the ossicles to suddenly return to their normal positions, causing the round window to implode
Barotrauma of the Ear
Most common complication of HBOT
It is inherently more difficult to inflate the middle ear because the inner ends of the Eustachian tube (fossae of Rosemueller in the naso-pharynx) have slit-like openings. These openings tend to close tighter if they are not open actively.
If the patient has descended more than about one meter without clearing the ears, it will be impossible to voluntary open the tubes through swallowing, yawning, or doing the Valsalva maneuver
The chamber pressure will have to be slightly decreased to facilitate ear clearing
Contraindications
Relative
Viral Respiratory Infections
may worsen with HBO
reason to temporarily interrupt daily treatment of some chronic illnesses
some authors feel that acute viral infections are a contraindication to HBO therapy because they may be severely exacerbated
Uncontrolled High Fever
may predispose to O2 seizures
should be reduced before placing the patient in the chamber
Seizure Disorders
may increase susceptibility to O2 seizures
premedication (with diazepam) may be advisable
History of Middle Ear Surgery
for treatment of otosclerosis
a wire or plastic strut might be displaced if the patient cannot equalize pressure in the ears
tympanostomy tubes may be needed
Upper Respiratory Infection
may make it difficult for the patient to equalize pressure in the ears and sinuses
decongestants are indicated
Severe Emphysema with CO2 Intoxication
removal of the hypoxic drive may cause respiratory arrest
Previous Thoracic Surgery
surgical scarring may have produced air-trapping lesions
History of Spontaneous Pneumothorax
Absolute
Premature infants
O2 in premature infants can cause retrolental fibroplasia (fibrosis on the surface of the retina) blindness
HBO is contraindicated in premature infants
Full-term babies may be safely treated with HBO
Bleomycin
Bleomycin chemotherapeutic agent used to treat a variety of tumors including head and neck, lymphomas, and germ cell testicular tumors
Effects of HBOT + Bleomycin
Pulmonary toxicity
Bleomycin can cause pulmonary toxicity leading to interstitial pneumonitis and fibrosis.
Increased oxygen tension seems to accelerate this side effect.
HBOT may cause rapid pulmonary deterioration and result in fibrosis
Disulfiram (Antabuse)
Occasionally used to treat alcoholism
Inhibits metabolism of alcohol which leads to an accumulation of acetylaldehyde causing headache, nausea, dyspnea
Antabuse blocks the production of superoxide dismutase which protects the body from oxygen toxicity.
Contraindicated in conjunction with multiple HBO treatments.
Concomitant administration of doxorubicin or cis-platinum as chemotherapeutic agents for cancer
Effects of HBOT with Chemotherapeutic Agents
HBO and doxorubicin given together has caused death in rats
probably from cardiac toxicity
HBO may increase the cytotoxic effect of cis-platinum in the tissue of chronic wounds, inhibiting healing.
Any patient who has a non-healing wound and is receiving cis-platin will not be helped, and may be worsened by HBOT
Untreated pneumothorax
Complication during ascent phase of treatment
Air volume increases in the pleural cavity, doubling or tripling, as atmospheric pressure is approached
Effects of HBOT on Untreated Pneumothorax
Treatment after HBOT
If pneumothorax occurs in the multiplace chamber under pressure, it must be relieved surgically before decompression
If pneumothorax occurs in the monoplace chamber, a McSwain dart or other chest tube is made ready, the chamber is decompressed not taking longer than 1 min, and the chest tube inserted as the patient emerges
Indications
exceptional blood loss anemia?
Intracranial Abscess (anaerobes in there; most effective of treatments –i.e. the best indication).
Thermal Burns
Compromised Skin Grafts and Flaps
Osteoradionecrosis
(Radiation Tissue Damage – vasculitis – blood vessels reduce in number over time after radiation)
Refractory Osteomyelitis
Enhancement of Healing in Selected Problem Wounds, e.g. diabetic ulcers
Necrotizing Soft Tissue Infections, e.g. necrotizing fasciitis, myonecrosis
Clostridial Myonecrosis (Gas gangrene)
Crush Injury, Compartment Syndrome, and Other Traumatic Ischemias
CO Complicated by Cyanide Poisoning in Smoke Inhalation
CO poisoning or smoke inhalation
Decompression Sickness
Air or Gas Embolism
Effects of HBOT
Result From
Mechanical Effects
Increased Partial Pressure of Oxygen
Mechanisms
Increased Partial Pressure of O2
Effects
Decreases Surfactant Production (100% O2 decreases surfactant)
Oxygen inhibits enzymes involved in the synthesis of surfactant
may also inhibit the transport of surfactant to the alveoli
Gilder and McCherry (1974).
Suppresses Autoimmune Responses
There are some experimental results that suggest that HBO has a suppressive effect on both humoral and cell-mediated immunity
May improve Nerve Cell Regeneration
Decrease in Lipid Peroxidation
Lipid peroxidation
Free radical damage to lipid (cell) membranes
One of the main causes of tissue injury following reperfusion of hypoxic tissue
Absolutely oxygen dependent
Enhances Antimicrobial Activity (aminoglycosides)
Effects of HBOT on Antimicrobial Activity
enhances the activity of aminoglycocide antibiotics (only antibiotic proven to improve effectiveness with HBOT).
Hyperoxia enhances phagocytosis and white cell oxidative killing of bacteria
Effects on Blood Cells?
enhances the killing ability of white blood cells
by increasing oxygen tension (recall increase of superoxide)
Decreases platelet aggregation
Multiple hyperbaric therapies may decrease the hematocrit by suppressing erythropoietin.
Reduce EPO reduced HB production.
Improved Tissue Salvage in Burns
Effects of HBOT on Burns
HBOT must be started within 24 hour of the burn
preferably ASAP
Hopefully Diminishing the number of surgical procedures required.
reduces the length of hospital stay and therefore cost
Preservation of epidermal basement membranes
Decreases extravasation of fluid from wounds therefore decreasing fluid requirements during the first few days after thermal injury
Decreases edema
Improved Tissue Salvage in Crush Injury
An injury caused by direct trauma or pressure.
Damage related to crush injury can include laceration, open wounds, fractures, bleeding, bruising, compartment syndrome and others.
The primary insult is tissue trauma, ischemia, and cellular hypoxia.
Vasodilation in the tissue surrounding the injury
leads to increased edema and further vascular compromise leading to ischemia
compromises the tissues ability to prevent infections
Effects of HBOT on Crush Injuries
Diminishes the risk of infection
Enhances leukocyte killing of intracellular bacteria
Produces a vasoconstriction that reduces edema formation
Increases oxygen tension leading to greater capillary oxygen diffusion.
Improved Healing in Bone Repair
Osteomyelitis
When used according to guidelines, HBO2 is clinically efficacious and cost effective.
Effects of HBOT on Osteomyelitis
Induces fibroblast proliferation and collagen synthesis
Enhances osteoblastic and osteoclastic activity
Increases osteoclast activity in removing necrotic bone.
Improves aminoglycoside transport across bacterial cell walls (antibiotic synergy)
HBO promotes angiogenesis
increases leukocyte killing ability
Increases oxygen tension in tissue which enhances leukocyte killing of intracellular bacteria
Reduces Carbon Monoxide (CO) Toxicity (prevents CO from binding; doesn’t wash it out though)
Effects of HBOT on CO Toxicity
In addition Oxygen breathing at 3 atm provides immediate delivery of dissolved oxygen (6cc) into the plasma in an adequate amount to support basic tissue metabolism even while CO is significantly bound to hemoglobin
HBOT produces rapid dissociation of CO from hemoglobin
About CO
Competes with O2 for hemoglobin (Hb) binding sites carboxyHb (HbCO)
CO has 240X greater affinity for Hb than O2 (if you remove 20% of the O2 molcs from Hb, that is life threatening.).
Byproduct of combustion
coal, wood, oil, natural gas, cigarette smoking
Colorless odorless gas
Inhibits Clostridium perfringens (a true anaerobe)
Gram-positive anaerobic rod-shaped bacteria
Associated with penetrating wound contamination & anaerobic conditions
Thrives in tissues with low oxygen tension
Gas Gangrene
Necrotizing Fascitis
Exotoxins (secreted by gram + bacteria) : Alpha & Theta toxins
These destroy host tissues and inflammatory cells
Cause hemolysis
They suppress myocardial contractility
-don’t die of infection; die of toxemia – with amputation, they will be better by tomorrow because toxin production has stopped.
The Infection is characterized by:
severe myonecrosis, gas bubbles & red or purple skin bullae.
Microscopy/cytology
necrosis, gas bubbles, large Gram positive rods
High mortality
shock, renal failure, ARDS, multi-organ failure
treatment
HBOT (90min of 100% O2 at 3ATM) is not the primary therapy in Gas Gangrene and Necrotizing Fascitis.It should be used in conjunction with timely surgical debridement (first) and appropriate antibiotic therapy.
The adjunctive use of HBOT therapy usually decreases the extent of radical surgical procedures
Effects of HBOT on Clostridium Perfrigens
Increases tissue oxygen
reverses hypoxic environment
Detoxifies alpha toxin
within 2 hours of elaboration
halts tissue destruction process
Inhibits alpha toxin production
symptoms
multi organ failure
ards
renal failure
shock
associated diseases
Necrotizing Fasciitis
Note red-purple bullae in skin; doesn’t involve the muscle. Vs. pyomyocytis starts in muscle – you have to amputate.
Note necrosis (arrow heads) and gas bubbles (arrows) within tissue. Gas bubbles would produce crepitus on palpation.
about CP A
Increased Healing of Hypoxic Wounds
HBOT increases tissue oxygen tension
stimulates angiogenesis
Ex: Skin Wound Dehiscence Following Achilles Tendon Repair
Shows the appearance of the right iposterior heel area and the resulting wound following dehiscence of the suture line after Achilles tendon rupture repair. This particular procedure had been performed four month previously with breakdown of the suture line within the first two weeks post-op.
Additionally, transcutaneous oxygen measurements near the site of the wound clearly documented hypoxic regions of the soft tissue immediately adjacent to the edges of the open ulcer.
Unsuccessful attempts at secondary closure led to consideration for the application of hyperbaric oxygen (HBO) therapy.
Skin Wound Following HBOT20 Tx; 2.0 atm, 90 min.
Shows the completely healed area of the Achilles tendon repair now five weeks following the completion of HBO therapy. The patient received 20 HBO treatments at 2.0 atmospheres absolute for 90 minutes each with routine wound care and supplemental oral antibiotic therapy. The patient has excellent range of motion and is ambulating without difficulty.
optimizes white blood cell killing capacity
optimizes fibroblast proliferation and
(at granulation tissue’ collagen secreted by fibroblasts; important for epithelial growth)
No Reduction (increase) of Blood Flow in Hypoxic Tissues
Vasoconstriction does not occur in hypoxic tissue i.e. chronic skin ulcers
plasma is able to carry dissolved oxygen to areas where red blood cells cannot go
may also beneit hypoxic tissues
these tissues may receive proportionately more oxygen during HBO than without HBO
Reduces Blood Flow in Hyperoxic Tissues (shunt is preferentially towards the diseased segment – vasoconstriction here (the normal side which has become hyperoxic under these conditions0)
add 6CC - the other 20CC can go to the ischemic areas
HBO causes vasoconstriction
No damage to tissues from hypoxia
elevated PaO2 ( increased O2 dissolved in plasma) more than compensates for the reduction in blood flow
reduces blood flow to tissues
increases peripheral vascular resistance
reduces edema
Oxygen behaves like any other drug: too little is not enough and too much will cause harm
Exceeding 3 atm oxygen gives no advantage and increases the toxic effects
Clinical use of HBOT is generally limited to a maximal partial pressure of 3 atm oxygen
Mechanical
CO2 Retention in Tissue
interstitial lung disease are seen as hypoxemia not hypercarbia - co2 easily diffuses out.
Rarely causes any problem
slight pH shift to the acid side
Also CO2 is buffered by bicarbonate
CO2 dissolved and transported in the plasma to the lungs independent of Hb
CO2 is 50 X more soluble in the plasma than oxygen
While breathing hyperbaric oxygen, Hb remains fully saturated within the venous circulation, blocking CO2 transport by Hb to the lungs for expulsion
Increases Oxygen Solubility in Plasma
HBOT raises oxygen tensions 10 to 13x their normal level when the patient is breathing 2.8 atm oxygen
when 6 volumes percent (6 ml per 100 ml of plasma) of oxygen are dissolved in the plasma, it is capable of carrying enough oxygen to meet the needs of the body’s tissues without RBC’s
HBOT reduces bubble size in the bloodstream.
following diving accidents or the iatrogenic introduction of intravascular air
injecting with a syringe - can do up to 500mL of...and they still wont die. Not a problem until having pressure which pushes into venous blood....
6cc/deciL of 02 that goes into the venous blood
Relevant for Air Embolisms
magnitude of an embolism goes down by 2/3 in a chamber
pressure is crucial to therapeutic effect
At 5 atm a bubble is reduced to 20% of its original volume and 60% of its original diameter
The therapeutic effect is achieved through mechanical reduction in bubble size.
Gas Gangrene
Clostridium perfringens type a
HBOT will reduce bubbles & tissue pressure increased perfusion with decreased ischemia & pain
gas bubbles in tissue tissue distention decreased perfusion
Follows Boyle’s Law
volume is inversely proportional to the absolute pressure
Types
remember that atm is 2.5-3atm.
IN a deciL of blood (100mL?)=20cc of Oxygen. = 5L of blood - has 1L of OXygen bound to Hb in the body. Note that none is dissolved into blood.
We extract 6cc of 02 per decil from arterial (33%)
At 3atm, 100% o2, 6CC will dissolve into plasma - that allows us to support ourselves without any oxygen from Hb, within the HB chamber.
n the lung between the alveolar wall and capillary wall is the interstitial space. (got to go through alveolar, capilarry and RBC cell wall).
People xposed to 50% oxygen have....interstitial space is permanently expanded - now need to be on 100% oxygen.
Oxygen of atm was 21%; we're making 100%.
21%02
we put 100% at 10lL/min
1l/breath 1 breath per sec
0L/min=10000cc/sec
166cc = max benefit
+210 in rm air = 38%
Without intubation, nobody gets more than 50% oxygen. Must be intubated and in a hyperbaric chamber.
Without intubation, nothing is dissolved in plasma.
Cant force it to dissolve in plasma without pressure.
add 6cc, the other of 20cc can go to hypoxic tissues
Toxic
Therapeutic